The alarmingly sharp increase in type 1 diabetes mellitus incidence in recent years has been coupled with a marked rise in the development of closed-loop systems aimed at continuously monitoring blood glucose levels, predicting glucose behavior and delivering adjusted insulin doses. However, to date, these systems still fall short of ensuring tight glycemic control in many patients, particularly in patients with high glucose variability. The presented clinically optimized blood glucose prediction technology, developed at the Weizamnn Institute of Science, provides for improved prediction accuracy, regardless of patient age and disease severity, and outperforms standard models, particularly in high-risk patient populations. The technology can be easily integrated into existing artificial pancreas systems and bears the potential of enhancing disease management and patient quality of life, translating to the long-term clinical benefits of stable glycemia.
The past decade has witnessed a considerable increase in the incidence of type 1 diabetes mellitus (T1DM) worldwide, particularly among young children. Intensive T1DM therapy is associated with high risk of hypoglycemia and weight gain and demands significant self-management competence. The development of the artificial pancreas, comprised of a continuous glucose monitoring (CGM) device, coupled to infusion pumps via dedicated dosing algorithms, has enabled more patients to meet their glycemic goals. However, overall, these closed-loop systems still provide relatively poor predictions, largely due to their development and training with medical logic and simulator-derived data (rather than actual data derived from patients), which fail to accurately integrate the numerous real-life factors impacting glucose levels.
The technology developed by this research group involves a clinically optimized blood glucose prediction algorithm with reduced error rate. Its development leveraged machine-learning computational tools and over 1.5 million glucose recordings collected from 141 T1DM patients simultaneously using a CGM and insulin pump. The model integrated a novel gradually connected network (GCN) in place of the standard artificial neural networks, which proved to be highly suitable for continuously acquired data. The algorithm demonstrated high accuracy, with similar performance for patients of different age groups and from a range of degrees of glycemic control. Moreover, it outperformed the autoregressive model in cases of high-risk patients spending a large percentage of time in hypoglycemia and in patients with high blood glucose variability.
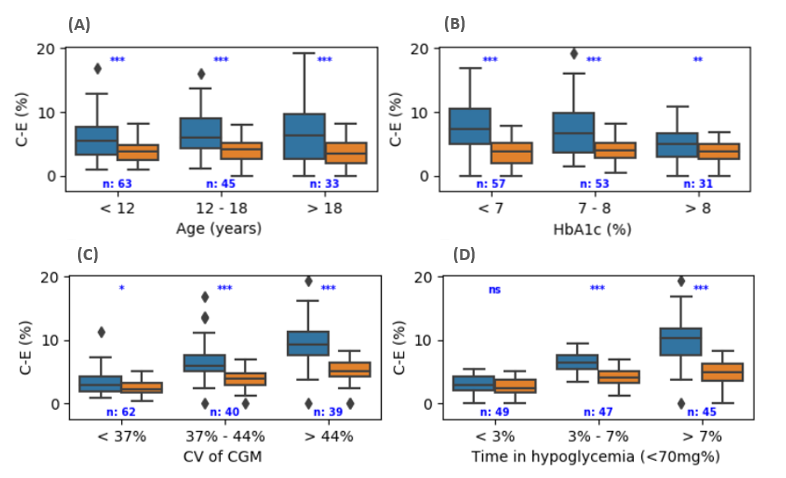
Comparison of performance of GCN3 model (orange) compared to the autoregressive model (blue) in patients of (A) different age groups, (B) different baseline hemoglobin A1c (HbA1c) values, (C) glucose variability and (D) percent of time in hypoglycemia. Shown is the percentage of predictions falling in clinically hazard zones (C-E) on the Clarke Error Grid (CEG) for all tested patients. From: Diabetes Technol Ther. 2020, 22.
Advantages
- Trained and tested using massive volumes of real-life data
- Accurate in broad, heterogeneous patient populations, including high-risk populations
- Prediction horizon of up to 60 minutes
- Smartphone-compatible
- Compatible with standard closed-loop system components
- Easily implementable
Applications
This invention can be integrated in standard closed-loop artificial pancreas systems comprised of a continuous glucose monitoring device and an insulin pump.
The novel blood glucose prediction algorithm has demonstrated high accuracy when tested with real-life, heterogeneous clinical data (Published in: Diabetes Technol Ther. 2020, 22). Ongoing work is optimizing the technology by incorporating additional clinical factors that impact glucose homeostasis, e.g., physical activity and meal content. A patent application was submitted for this technology.
An estimated 1.25 million Americans have T1DM, with approximately 40,000 new cases diagnosed each year in the United States alone. Recent years have seen a significant increase in incidence rates, particularly among young children. The demonstrated efficacy of artificial pancreas closed-loop systems, along with the convenience and improved confidence they provide patients and caregivers, have brought to a marked increase in the market value of CGMs and insulin pumps. Between the years 2011 and 2016, CGM use among children under 6 years of age sharply rose from 4.4% to 44.5%. Its 2018 total market value was $575 million and its overall CAGR from 2019 through 2025 is expected to be approximately 13% reaching around $1.3 billion by the end of this time period. In parallel, the global insulin pump market size is expected to reach a valuation of 8.5 billion USD by 2023 with a CAGR of 8.4% between 2017 and 2023.

Dr. Vered Pardo Yissar

