5629
Overview
Subdural hematoma (SDH) is a common neurosurgical condition that requires continuous monitoring, which current imaging methods fail to provide.
TOVA is a wearable device that combines radio frequency (RF) and optical sensing technologies to provide continuous, precise SDH monitoring through the intact skull.
Applications
- Continuous monitoring of SDH during hospital stays and post-discharge
- SDH detection and monitoring in ambulances and urgent care settings
- Long-term monitoring in various care facilities (nursing homes, community clinics)
- Identification of brain asymmetry and intracranial pressure
Diffrentiation
- Continuous, real-time monitoring of SDH expansion
- Early detection and alerts for hematoma expansion
- Simple, low-cost production, with simple operation not requiring specialized training
- Detection of hematomas as small as 1 cm
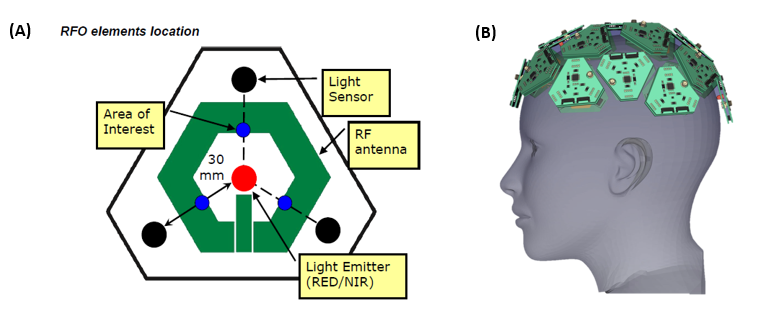
Sensor design (A) and assembly (B)
Development Stage
The technology has been successfully tested using a single sensor element in mice and human head phantoms. A lab-stage prototype is under development, with further testing planned. Multiple patents have been granted (European, and multiple US patents).
Patent Status:
USA Granted: 11,540,725 USA Granted: 11,395,590 USA Published: Publication Number: US 2025/0000435 A1
Contact for more information

Dr. Vered Pardo Yissar
Senior Director of Business Development, Exact Sciences

